
When the Therapist Becomes the Parent: Lessons Learned During our NICU Experience

I stood at my daughter’s bedside and told the nurse, “It’s so much information. I don’t understand. They had me signing consent forms for procedures that outlined the risks, but I still didn’t feel like I completely understood them. It’s like I need to hear everything half as fast and twice over. If it wasn’t my child, I could keep up, but it’s so different when they are talking about your baby.”
My daughter was diagnosed with Pierre Robin sequence and Stickler syndrome and spent 7 weeks in the NICU due to micrognathia, glossoptosis, and a cleft palate. I shared her NICU journey, progress, and surgery on my speech therapy Instagram account. I received messages throughout our NICU stay from SLPs and other service providers expressing gratitude for sharing our experience and saying it was helpful to see things from the “other side.” As I received requests to hear my learned insights and advice for service providers, I decided to write this all down in a more formal and cohesive form!
First off, I want to share something I posted on social media the day my daughter came home from the hospital. I feel it represents where my head and heart were at that moment:
“Time and time again, I have thought how grateful I am for those who have dedicated their lives to becoming knowledgeable in an area that could help my baby in a particular moment – the peds ENTs, SLP, OT, PT, neonatologists, nurses, dietician… Countless people were critical in getting her to the point that she could come home. This little girl has come a long way from not being able to breathe or eat independently, and we couldn’t have asked for a better outcome.”
I hope my perspective can help the NICU SLPs, OTs, PTs, and other providers. I have also incorporated into my insights what dozens of fellow NICU parents in my social media audience shared about their experiences.
All these thoughts are based upon being in the NICU, but I saw parallels that could benefit me and others while working in different settings.
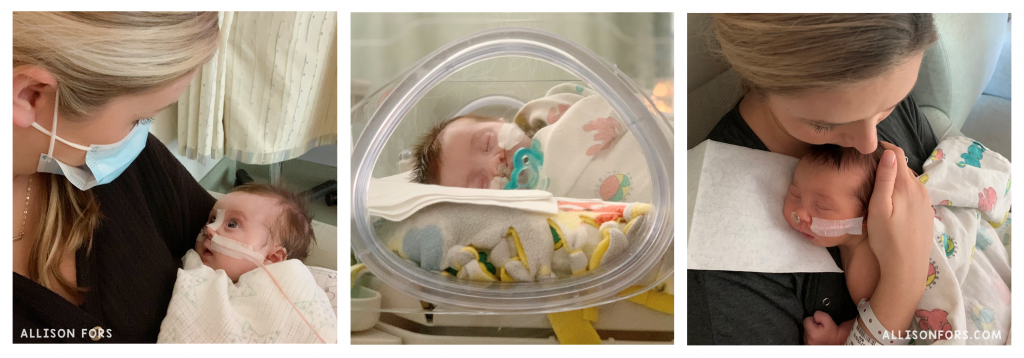
MY LEARNED INSIGHTS AND ADVICE AS A NICU PARENT
Be sensitive and supportive.
This is the most critical piece of advice I have to share. Having a baby in the NICU is an incredibly difficult time in these parents’ lives. If you take anything away from this post, let this be it! In talking to other NICU moms, there was the repeated sentiment that this was one of, if not the hardest, periods of their lives and a time where they felt so alone.
And this is the period of time you are interacting with these parents!
Be overly sensitive and supportive! Grieving is taking place in many forms. It was continually evolving for me throughout our 7-week NICU stay. Be gentle. I have never been more sensitive and emotionally drained. It was challenging to cope with even the smallest negative interaction. Being in a hospital and the NICU is typical for you but very scary and foreign for us. On the same note, forgive the parents quickly and often – sometimes we aren’t acting rationally because of the stressful nature of everything.
Our OT was great about this. Every time she was about to leave, she would make sure to ask if I needed anything. She would bring water or a stool for my feet. It was those tiny things that helped. And remember, these moms just gave birth! Three days after my C-section, they had me hold my daughter down for over an hour trying to get an IV in her and my body couldn’t handle it.
It is easy to become jaded in any profession. Take a step back and put yourself in the parent’s position – their baby is in the hospital, their child just received an autism spectrum diagnosis, or your elderly patient just learned they can’t eat solids! No matter what settings you work in, make a conscious effort to put yourself in their shoes. This experience is still so fresh for me, but I hope that it will always help me be more empathetic with those I work with going forward.
Talk slow and repeat everything. Ask if they have questions.
Everything is more challenging to comprehend when it’s your child and the emotional element is there. This took me a couple of weeks to piece together. I was frustrated with myself for not being able to keep up in conversations or ask the right questions in the moment.
My husband is a doctor who understands the medical talk, and I had a leg up on all the feeding aspects of her intervention with my speech background. Even then, I felt I was struggling to follow along.
When the SLP came the first time (and didn’t yet know that I have a background in speech) and started talking about “aspiration” and “epiglottis,” I knew what she was talking about, although most parents would have been completely lost.
Another time I got a call in the middle of the night from the doctor using terminology I didn’t know and giving me numbers that I had no basis for knowing what they meant. And he wanted me to base the decision of giving her a blood transfusion on these things!
The next day a different doctor slowed down and explained why he was recommending a blood transfusion. He used an analogy for what red blood cells were for and what they do. Now, I know the purpose of red blood cells, but I appreciated it because it gave me time to think of questions and form an opinion.
Remember, most of the terminology associated with your field is a foreign language to the majority of parents!
So…
Talk at half speed.
Repeat everything twice.
Then ask if they have questions. More than once!
Give them time to wrap their head around what you’re saying and time to think of questions. I know, time is always limited and caseloads are full – but just remember that under stressful situations, parents (and patients themselves) need more time in comprehending information.
Explain your role in simple terms and reintroduce yourself every time.
There were a lot of members on her team. We had different doctors, nurses, the SLP, OT, PT, dietician, lactation nurse, and others. There are so many people in the hospital; the nurses and doctors are constantly changing, so it can be hard to keep everyone straight. Usually, I’m good with faces and names! But I think due to this high-stress situation, my brain was not firing on all cylinders. When someone showed me their badge and I was able to see their name and role, it helped me remember them. Even if you think the parent remembers you, tell them your name and who you are again! One day I forgot who the PT was and we’d had multiple interactions by that point!
Don’t forget to explain your role in the ultimate goal of their child being discharged from the NICU – in simple terms! Visuals are ideal if you’re diving into any anatomy or physiology. I never received any handouts but requested them in regards to feeding babies with clefts. I think handouts would be helpful because parents are able to read and digest in their own time and refer back to them.
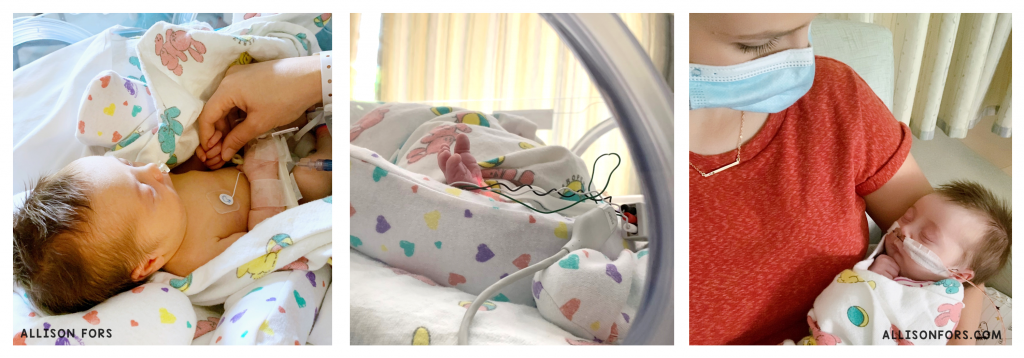
Help the parent have a role in their child’s care.
One of the significant mental hurdles when your baby is in the NICU is your inability to care for your child. I could pump milk for her, change her diaper, take her temperature, and that was it. She didn’t even really feel like my baby, and I struggled with the thought if she even knew I was her mom.
Try your hardest to include parents in firsts! Firsts are a big thing for parents, especially first-time parents. Little things like the fact that I didn’t bathe or dress my daughter until she was home at 7 weeks old were difficult!
I went to the NICU to visit my daughter the day after she was born. The nurse told me I couldn’t hold her but didn’t explain why. She then proceeded to stand between my baby and me to do things I could have done for her – like changing her diaper. This crushed me. I didn’t even see my daughter until she was 8 hours old, and this was my second time seeing her ever. That one-minute interaction with the nurse could have gone so differently by just offering a quick explanation, even if it meant I still couldn’t hold my baby. I heard from many parents that they felt in the way or that they were annoying the staff.
Part of making a parent feel part of their child’s care is also providing them that extra support so they feel like they have the skills to do things for their child. We were able to introduce a bottle when my daughter was 6 weeks old. Due to COVID-19, my husband and I couldn’t be in the NICU together. He was initially the one there when the therapists trained us on how to use the specialized bottle. The first time I gave her a bottle they just watched, and it was overwhelming! I felt incompetent for the first few days of bottle feeding. Nothing is more defeating than feeling that can’t take care of your own child. Providing extra support and encouragement goes a long way. It is a strange feeling never being alone with your baby and having everything be watched!
The parent’s opinion deserves a spot at the table.
This one feels strange to add because I know there are plenty of caveats, but I feel it’s necessary because I heard many stories from fellow NICU parents when this was an issue. As the trained professional, you have much more information and experience compared to parents, but it is critical to have parents feel heard.
Parent intuition should be valued (of course to a reasonable degree.) Sometimes things can’t be entirely explained by logic, and you have to trust your gut as both a parent and a provider. You also need to trust the gut of the patient’s family. The last thing NICU parents need is to feel like they are being brushed off and treated like an overly-emotional parent. Let them feel heard and take their opinion or concern into account.
A time when I experienced this firsthand was one of the hardest NICU days. I knew something was wrong, but I had to be so aggressive and persistent to get something done about it:
One day my daughter was working hard to breathe and the monitors were continually beeping as she desaturated repeatedly. (She breathed via a nasopharyngeal airway, also called a nasal trumpet – a tube that went into her nose and back behind her throat, which opened her airway. Nasal trumpets are fairly uncommon and many nurses and doctors were uncomfortable caring for and changing it.) No matter how I held her or what I tried, it was still an issue. The only thing left was to assume that the trumpet was occluded from hardened secretions and reflux. The nurse did not think this was the case since nothing came out when she suctioned it. I knew from previous experience that it could still be occluded even if the suction came back clean. Despite constantly voicing my concern, she wouldn’t change the trumpet or call the doctor to do it. The break nurse did listen to my concerns and agreed something was wrong with her breathing. She called the doctor, who proceeded to suction and try everything we already did and tell me the trumpet was fine. It took me about 30 minutes to convince him to change it. After hours of persistently asking and begging (and eventually telling), it was finally changed. And sure enough, it was occluded. You could even see the hole that the suction catheter poked through the occlusion, and that’s why it kept coming back clean. There was no logical explanation as to why she wasn’t breathing well, and it didn’t necessarily point to the trumpet as the issue.
But it was the issue.
It was difficult for me to be bold in this situation, and it made for a beyond awkward day, but what would have happened if I hadn’t pushed!? And guess what…that doctor and I had excellent rapport after that and he ended up being one of my favorite doctors!
(Funny side note: Weeks later, a nurse said, “I heard about the time her trumpet was occluded, and you were the only one that wanted to change it.” I guess the story got around!)
Now of course there are times when the parent’s opinion is incorrect, and navigating that deserves a blog post of its own. Certainly we should resist any influence that would hinder a patient’s care. But I think if the parent presents an opinion that isn’t unreasonable, it should be given consideration. And undoubtedly the intervention will be more successful when parents feel like they are involved in the care.
Information is bound to get lost with carryover and patient hand-offs.
Carryover is a common roadblock in all settings – teachers, aides, parents…
In the NICU this happens a lot since there is a constant changing of caregivers between the nurses and doctors. It’s inevitable, but there are ways to mitigate the damage. We had the feeding therapist put step-by-step directions of exactly how to feed her on her bed, and even then, there were times when I’d walk in and she was being fed incorrectly. Nurses are used to doing things a certain way, which works well for them most of the time! As a parent, this was frustrating because I felt like I was playing the middle man and trying to convince or teach the nurses.
Information is bound to get lost in hand-offs, but do everything in your power to limit the amount and to make it as easy as possible for the others involved to follow the care plan you have put in place. Incorporating clear written instructions, a communication order in the EMR, or some other process that your institution uses makes a difference.

THE BACKGROUND: COMMON QUESTIONS
What surgery did she have?
She had a mandibular distraction surgery at 4 weeks old. The jaw distraction pulls the lower jaw forward, opening the airway and bringing the tongue forward. This allowed her to breathe for the first time on her own! Before the surgery, my daughter was unable to breathe on her own or swallow. She breathed using a nasal pharyngeal airway (nasal trumpet) and fed using an NG tube.
Does she need more surgeries?
She will need another surgery to remove the hardware in her jaw from the mandibular distraction. This typically occurs a few months after surgery. She will also have the cleft palate repair done when she is closer to a year old.
Did you know she had a cleft palate before birth?
We didn’t know she had a cleft palate while I was pregnant, but we suspected it. We knew she had a small jaw that had the potential implications of impacting breathing and is often associated with a cleft palate. When the jaw is small, the tongue gets pushed back and up, impeding the proper palate closure. While a cleft lip is easily detectable on ultrasound, it’s challenging to see a cleft palate.
In addition, Stickler syndrome runs in my husband’s family, and the small jaw was a good indication she had the genetic disorder. We were not anticipating the severity of her case since those affected in the family are more mild cases, not exhibiting the breathing issues or need for surgery.
How is she doing now?
Great! There are no issues with breathing nor her oxygen levels since the surgery. Feeding is the biggest struggle, which is very common in cleft palate babies. She gets tired quickly during feeds and has a hard time getting enough food. This is because she can’t create proper negative pressure to draw milk from the bottle, but by fortifying her bottles with extra calories she is gaining weight.
Will she need any intervention as she grows?
She will most likely need speech therapy for articulation errors. There is also a good possibility she will have some level of hearing loss. She may need the same jaw distraction surgery as a teenager if her jaw doesn’t grow enough.
I know our NICU experience has given me a newfound respect and compassion for parents, and no doubt will change how I interact with parents in the future. I hope this post in some way helped you understand “the other side.” Know that you are providing an amazing service for these kids and their families!

You may also be interested:
The Importance of Explaining the WHY of Therapy to Parents
Cleft Lip and Palate





One Response
Thank you for sharing. I will keep this all in mind while serving my elementary kiddos, especially during distance learning where many parents are overwhelmed.
Thank you.